Healthcare foodservice operations continue to adjust to a recalibrated normal as states lift restrictions that were in place to slow the spread of COVID-19.
“We’ve all learned about patience and resilience,” says Martha Rardin, MS, RD, CD, FAND, director of Nutrition and Dietetics at Hendricks Regional Health in Danville, Ind. “At first it was mind-boggling how problems outnumbered solutions. Things were changing nonstop, rapid-fire for months. We discovered we are far more resilient than we might have thought.”
Staffing continues to challenge most foodservice operations. “Staffing relative to volume and hours of service is now better understood and can be managed perhaps more quickly by knowing the minimum necessary to run an operation and which operations are essential,” says Georgie Shockey, owner and president, Ruck-Shockey Associates Inc., Spring, Texas.
 Popular customized salads are back at Robert Wood Johnson University Hospital.
Popular customized salads are back at Robert Wood Johnson University Hospital.
Patient Services
Tray delivery to patients has largely returned to pre-pandemic modes of operation, including china service. At Edward-Elmhurst Health in Illinois, Dave Edwards, system director, and his team have resumed passing trays to all patients. From March 2020 to January 2021, the team left trays just outside COVID-19 patients’ rooms so nurses could deliver the trays. “This significantly reduced the impact on nurses,” Edwards says.
 Nick Tetreault oversees the salad bar at at Riverside Regional Medical Center. Some changes made to slow the spread of COVID-19, though, could become more permanent. For example, the approach taken for serving food to patients in isolation. Prior to COVID-19, protocol for serving isolated patients at Robert Wood Johnson University Hospital (RWJUH) in New Brunswick, N.J., was to serve patients food products on regular trays and dinnerware. “During the pandemic, all COVID patients and isolation patients were served their meals on disposables," says Jill Wedeen, MPA, RD, assistant director, Clinical Nutrition and Patient Service, “which will now become a permanent practice for all of our isolation patients.”
Nick Tetreault oversees the salad bar at at Riverside Regional Medical Center. Some changes made to slow the spread of COVID-19, though, could become more permanent. For example, the approach taken for serving food to patients in isolation. Prior to COVID-19, protocol for serving isolated patients at Robert Wood Johnson University Hospital (RWJUH) in New Brunswick, N.J., was to serve patients food products on regular trays and dinnerware. “During the pandemic, all COVID patients and isolation patients were served their meals on disposables," says Jill Wedeen, MPA, RD, assistant director, Clinical Nutrition and Patient Service, “which will now become a permanent practice for all of our isolation patients.”
In response to staffing reductions as well as shortages of menu items, many hospitals also reduced menu variety, while others looked at patient and retail menus through a more holistic lens than before. At Ohio State Wexner Medical Center in Columbus, for instance, Julie Meddles, MS, RDN, LD, director, System Nutrition Services and gift shops, and her team started to design recipes that incorporate menu ingredients that can be used in patient foodservice as well as retail operations. For example, they developed a meat sauce, which they prepare and chill in the production kitchen, for use in multiple pasta dishes. They also purchase the same sandwich buns for patient and retail menus to enhance efficiency of ordering and storage.
“Since the pandemic began, retail operations were most impacted in terms of sales dropping,” Shockey says. For months, many retail operations shut down completely while others worked with minimal services in response to state restrictions and low employee and visitor participation.
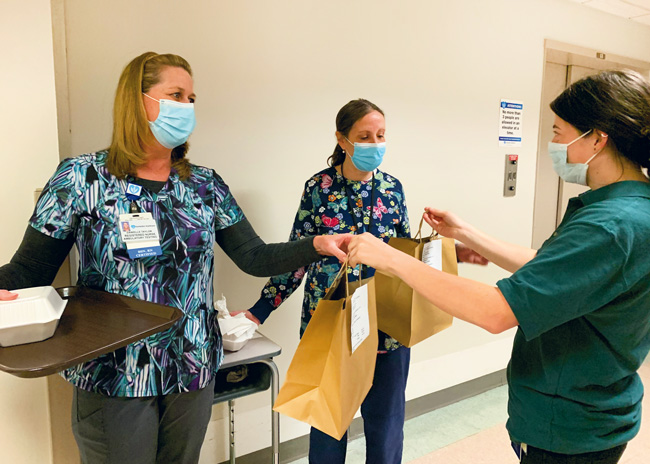 Staff pass mobile orders to hospital employees at Hunterdon Medical Center.
Staff pass mobile orders to hospital employees at Hunterdon Medical Center.
Self-Service vs. Served Foods
“Self-service is coming back to many locations for at least at a station or two,” says Shockey. She adds that staffing issues will likely not allow full service in all areas.
At Morrison Healthcare-contract managed hospitals in Chicago and St. Louis, dining staff turned self-service salad bars into staff-served salad bars or designated an area where customers can choose prepackaged salads. “In some hospitals, salads are offered at deli concepts or other stations,” says Laurie Schutter, MBA, regional vice president, Morrison Healthcare, a division of Compass Group North America. At some stations, customers can select ingredients such as diced chicken and vegetables packaged in condiment cups to customize their own salads.
Though employees at RWJUH still can find prepared to-go salads in containers, every week they can purchase a different staff-prepared salad at a designated action station. All other retail stations are up and running as well. “We’re offering display cooking and all the menu items, including sushi on Fridays,” says Tony Almeida, DHCFA, director of Food and Nutrition.
Riverside Regional Medical Center in Newport News, Va., on the other hand, reports opening its salad bar in October 2020. A team member watches over the salad bar every moment it is open. Due to labor constraints, this
area operates with limited hours, from 11 a.m. to 3 p.m. Monday through Friday, instead of 11 a.m. to 7 p.m. daily as it did before the pandemic. As things progress, Riverside Regional may expand the hours of operation for its salad bar and bring back the fruit/yogurt bar in the mornings.
The salad bar’s return required a couple of operational updates. When customers approach the salad bar at Riverside Regional, they use hand sanitizer and put on gloves before moving along the bar and making salad selections. Staff replace utensils at least once an hour. When customers reach the end of the bar, they take off the gloves and place them in a trash container.
The selection of menu ingredients, such as nuts and sunflower seeds, was reduced slightly but may increase in coming months. Individual packets of salad dressings replaced shared-use bottles of dressings. “These salad dressings are more expensive, but we don’t have to worry about contamination of lids and the bottles themselves,” says Antoinette “Toni” Watkins, MS, RDN, system director of Food and Nutrition Services, Riverside Health System.
Overall, the return of the salad bar has been very well received. “You would have thought we were giving away gold when the salad bar opened,” Watkins says. “Who would have thought a salad bar would have been such a satisfier for team members.”
Since Riverside Health brought back its salad bar last fall, it has sold roughly 1,900 salads a month in an operation serving about 25,000 customers a month, says Nick Tetreault, retail manager at Riverside Regional Medical Center. “Many of our customers exclusively eat from our salad bar so they were ecstatic to see it available again. Pre-pandemic, we were selling roughly three to four thousand salads a month,” he says. “We’re seeing an uptick in the number of transactions so we can see we are heading back toward our typical numbers.”
“There is still a slight apprehension for many when it comes to self-serve stations and dining in public,” Tetreault says. “But I feel confident in the safety and sanitation measures we have implemented to ensure that customers can make themselves a fantastic salad and stay safe at the same time.”
 Leg Up supplies grocery items for the minimarket at WellSpan-York Hospital.
Leg Up supplies grocery items for the minimarket at WellSpan-York Hospital.
Grab-and-Go and Minimarkets
Many hospitals report an unprecedented rise in the number of grab-and-go menu items and cashier-less payments.
 Customers find mobile app orders at BistrOH! To Go and other locations at Ohio State Wexner Medical Center.Morrison Healthcare’s Schutter says to-go menu service increased exponentially in many of the company’s contract-managed hospitals. One of the most popular offerings are take-home meal kits that caregivers pick up in the retail area before they leave work. Named Fresh Easy Delicious (FED), the take-home kits include chopped and measured ingredients along with a recipe for such items as pasta bakes, premade salads and pizza.
Customers find mobile app orders at BistrOH! To Go and other locations at Ohio State Wexner Medical Center.Morrison Healthcare’s Schutter says to-go menu service increased exponentially in many of the company’s contract-managed hospitals. One of the most popular offerings are take-home meal kits that caregivers pick up in the retail area before they leave work. Named Fresh Easy Delicious (FED), the take-home kits include chopped and measured ingredients along with a recipe for such items as pasta bakes, premade salads and pizza.
A popular service Schutter and her Morrison Healthcare and Compass Group colleagues restarted live in late June are the interactive demonstrations in the facility’s teaching kitchens. “For several months in response to COVID, Morrison Healthcare offered a virtual teaching kitchen, which allowed our guests to explore food, culinary and nutrition literacy without leaving the comfort of their own kitchens,” Schutter says. The company continues to host a site dedicated to wellness and sustainability. In addition, Schutter’s region offers a mobile teaching kitchen that staff bring to hospitals to provide wellness support.
Concerned about caregivers working around the clock to support the needs of very ill patients, administrators at WellSpan Hospitals in Pennsylvania make their employees’ lives a little easier. They set up small markets, which are partnerships with small, independent grocery stores or farmers in the region, for team members to access in the hospitals. “Staff were — and still are sometimes — so stressed, and this is one less stop on the way home,” said Tim Bentzel, senior director of Food and Nutrition Services for WellSpan Health.
A market has become a permanent fixture at WellSpan York Hospital in York, Penn., stocked with products from Leg Up Farmers Market, located 10 miles north of the hospital. The hospital provides the space and minimal staff support for the miniature market. Leg Up, which specializes in selling locally grown and sustainable food, brings in and sets up the groceries, including home replacement meals and staple supplies. Employees can purchase the items at cost. “We aren’t making a profit but rather are offering a service,” says W. Michael Long, director, Food and Nutrition Services.
The 20-foot-by-20-foot market, which sits adjacent to a coffee shop near the atrium lobby, contains refrigerated and ambient display cases, shelving and tables. Customers pay the cashiers working at the coffee shop. The market operates at the same hours as the coffee shop, from 7 a.m. until midnight.
“The grocery items weren’t moving as much as we expected, so we expanded our service model to also include a grocery/delivery drop-off service in which customers place orders on Leg Up’s website,” Long says. “This gives them access to a full line of Leg Up products in addition to the items displayed in our market.” Leg Up delivers the packaged orders along with grocery items to the hospital’s market three times a week. Customers find their packaged orders in a designated reach-in display cooler.
 Celebrity chef Bal Arneson, a Morrison Healthcare partner, shares stories about food with children participating in the teaching kitchen at a hospital.
Celebrity chef Bal Arneson, a Morrison Healthcare partner, shares stories about food with children participating in the teaching kitchen at a hospital.
Ordering Apps and Delivery Services
Many operators use mobile ordering apps. “With our mobile ordering app developed by Morrison Healthcare, we saw a large increase in takeout services,” Schutter says. About one-third of the hospitals in Schutter’s region offer app ordering.
At Ohio State Wexner Medical Center in Columbus, Ohio, medical center employees also can order through a mobile app and pay via payroll deduct, credit cards or Apple Pay.
Angela O’Neill, director of Nutrition Services, Hunterdon Healthcare in Flemington, N.J., and her team introduced a delivery service named E-Cafe2U. Customers order on a supplier-developed app and pay via payroll deductions. They receive notification when their menu items arrive at one of 14 delivery stations. The service appeals to employees who work in areas they can’t leave during meal periods; staff also like the menu variety and some use the service to take food home for dinner.
Delivery service takes place 7 days a week and attracts new customers who weren’t coming into the cafeteria and therefore creates additional revenue. Check averages are higher than in the cafe because customers are selecting add-ons. The goal is 50 orders per weekday and 20 per weekend day. In June, they had reached 60% of their goal.
Geisinger in Pennsylvania implemented a supplier-developed ordering app at all eight of its healthcare sites. Customers place orders for pickup at a specific time. The kitchen staff prepare the orders and place them on a rack near the cashiers, who monitor the rack. Employees and visitors pay directly through the app via the payroll deduction system or with credit cards. “We promoted this early in the pandemic and amped it up as we went along,” says Lynne C. Brown, operations director, foodservice, Geisinger, Wilkes-Barre, Penn.
App ordering has helped the Geisinger foodservice staff deal with staffing shortages at one operation and will soon be in effect at others. “Staffing shortages have been a nightmare,” Brown says. “With app ordering, we closed one retail operation after 2 p.m. and on weekends.” With app ordering, customers can still order food, which staff make in the kitchen and package with the customer’s name on the label and place on a rack for pickup.



